Living with lupus can feel like navigating an unpredictable storm. Symptoms come and go, affecting different parts of the body in unique ways. While medical treatments are essential, holistic approaches and proper nutrition can offer a powerful way to manage symptoms and improve quality of life. Understanding how specific dietary choices and lifestyle adjustments influence lupus can empower individuals to take control of their health.
The Impact of Lupus on the Body
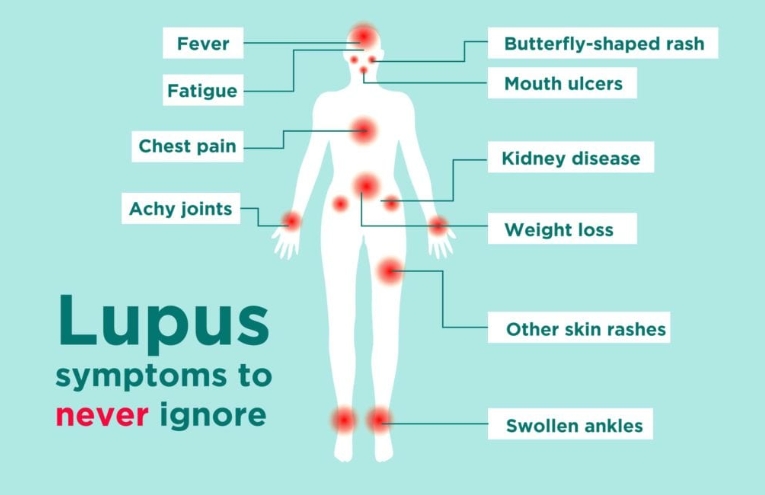
Lupus, or systemic lupus erythematosus (SLE), is an autoimmune disease where the immune system mistakenly attacks healthy tissues, causing inflammation and damage. The effects vary, but common areas impacted include:
Joints and Muscles: Many people with lupus experience joint pain and stiffness, often in the hands, wrists, and knees. Muscle aches can also add to the discomfort.
Skin: The classic “butterfly” rash across the cheeks and nose is a hallmark sign, but lupus-related rashes can appear elsewhere and may worsen with sun exposure.
Kidneys: Lupus nephritis, an inflammation of the kidneys, affects about half of those with lupus, potentially leading to swelling and high blood pressure.
Heart and Lungs: Inflammation can lead to conditions like pericarditis (inflammation of the heart lining) and pleuritis (inflammation of the lung lining), causing chest pain and breathing difficulties.
Nervous System: Headaches, dizziness, memory problems, and even seizures can result from lupus affecting the nervous system.
Blood and Blood Vessels: Issues such as anemia, increased clotting risk, and lowered immune function can occur due to abnormal blood cell counts.
The Role of Nutrition in Lupus Management
Diet plays a crucial role in managing lupus by helping to control inflammation and support overall health. While no one-size-fits-all diet exists, certain foods have been found to be beneficial:
Mediterranean Diet: This diet, rich in fruits, vegetables, whole grains, lean proteins, and healthy fats, has been linked to reduced inflammation and cardiovascular risk in lupus patients.
Omega-3 Fatty Acids: Found in fatty fish like salmon and mackerel, omega-3s help reduce disease activity and inflammation.
Vitamin D: Many with lupus are deficient due to sun avoidance. Supplementing vitamin D can support bone health, immune function, and energy levels.
Fruits and Vegetables: Packed with antioxidants, these foods help combat oxidative stress and inflammation.
Foods to Avoid: Alfalfa sprouts contain an amino acid (L-canavanine) linked to lupus flares, and some people find that nightshade vegetables (potatoes, tomatoes, eggplant) exacerbate symptoms. Processed and sugary foods can also contribute to inflammation.
Holistic Approaches to Managing Lupus
Beyond diet, lifestyle adjustments can play a major role in reducing symptoms and improving daily life.
Physical Activity: Low-impact exercises like walking, swimming, and yoga can improve joint health and reduce stress without overburdening the body.
Stress Management: Mindfulness meditation, deep breathing exercises, and engaging in hobbies help lower stress levels, which can trigger lupus flare-ups.
Adequate Rest: Prioritizing sleep and listening to the body’s needs can help manage fatigue.
Support Systems: Connecting with others who have lupus, whether through support groups or online communities, can provide emotional and practical support.
Mind-Body Therapies: Practices like tai chi and acupuncture may help with pain relief and overall well-being.
Personal Stories of Resilience
Hearing from those living with lupus offers inspiration and insight into effective coping strategies.
Caragh Keane: Diagnosed at 25, Caragh struggled with severe joint pain and fatigue. Through dietary changes focused on anti-inflammatory foods, she saw major improvements and went on to create Superkeen Foods to help others with similar health challenges.
Muni Long: The Grammy-winning singer has managed lupus since 2014. She tailors her lifestyle to accommodate her health needs, emphasizing self-advocacy and stress management.
Emerging Research: Peptide-Based Therapies
New treatments are being explored to manage lupus symptoms more effectively:
P140 Peptide (Lupuzor): A promising therapy that modulates the immune response and has shown potential in reducing disease activity.
Blisibimod: Targets B-cell activating factor (BAFF) to help regulate immune function.
Efavaleukin Alfa: An experimental drug designed to boost regulatory T cells, which play a crucial role in maintaining immune balance.
Managing Nerve and Skin Irritation
Lupus often causes skin and nerve-related symptoms, which can be managed through a combination of medical treatments and lifestyle adjustments.
Topical Treatments: Corticosteroids and antimalarial medications like hydroxychloroquine can help manage skin flares.
Sun Protection: UV exposure can trigger symptoms, making daily sunscreen use and protective clothing essential.
Neuropathy Management: Pain relief strategies include physical therapy, medications like NSAIDs or anticonvulsants, and lifestyle modifications.
Smoking Cessation: Quitting smoking has been linked to improved skin health and overall disease outcomes.
Conclusion: Embracing a Holistic Lifestyle
Living with lupus is challenging, but a combination of medical treatments, proper nutrition, and holistic approaches can make a significant difference.
Start Small: Introduce one new habit at a time, like a daily walk or a five-minute meditation.
Listen to Your Body: Pay attention to how different foods, activities, or stressors impact symptoms.
Seek Professional Guidance: Work with healthcare professionals before making major dietary or lifestyle changes.
Celebrate Progress: Every small victory, whether a pain-free day or trying a new recipe, is worth recognizing.
By taking a well-rounded approach to managing lupus, individuals can create a lifestyle that supports both physical and mental well-being, leading to a more balanced and fulfilling life.
Chuck Walton
Shamrock Fit

