How Past Trauma Affects Fat Loss and Overall Health Understanding the Connection Between Trauma and Health
When we think about fat loss and overall health, we often focus on diet and exercise. However, past trauma plays a significant role in both physical and mental well-being. Undigested trauma can lead to hormonal imbalances, chronic inflammation, and metabolic dysfunction—all of which make it harder to lose fat and maintain a healthy body.
This article explores the physiological and psychological connections between trauma and health, examining key systems in the body and strategies for healing beyond mental health counseling.
Physiological vs. Psychological Connection
Trauma affects both the mind and body. While psychological trauma can cause anxiety, depression, and PTSD, it also has a direct physiological impact by altering hormone regulation, gut health, and immune function. The body stores trauma in the nervous system, leading to chronic stress and dysregulation of key bodily processes that influence fat storage and metabolism.

Hormone Regulation: Cortisol, Insulin, and Stress Response
Chronic stress from unresolved trauma triggers excessive cortisol production. Elevated cortisol levels can:
Increase fat storage, particularly in the abdominal area
Disrupt insulin sensitivity, increasing the risk of metabolic syndrome
Suppress thyroid function, slowing metabolism
Studies show that individuals with a history of childhood trauma have higher cortisol levels and an increased risk of obesity and metabolic disorders (Heim et al., 2008).
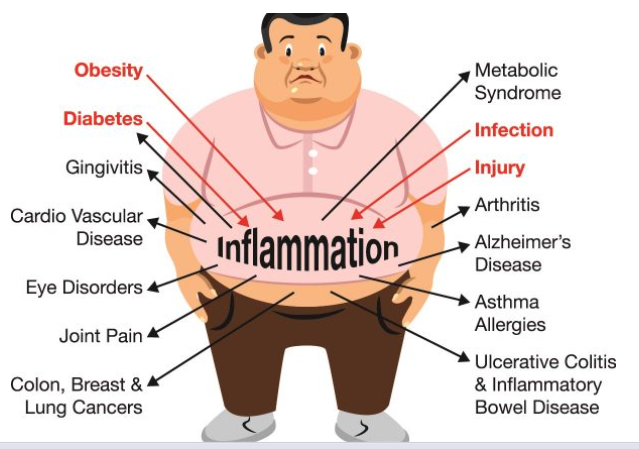
Inflammation and Gut Health
Trauma-induced chronic stress leads to systemic inflammation, contributing to weight gain and chronic illness. Elevated inflammatory markers, such as C-reactive protein (CRP), are linked to obesity and metabolic disease (Miller et al., 2011).
Gut Microbiome and Trauma
The gut microbiome plays a crucial role in digestion, immune function, and even mental health. Trauma and stress negatively impact gut bacteria balance, leading to:
Increased intestinal permeability (leaky gut)
Poor digestion and nutrient absorption
Higher levels of inflammation that contribute to fat storage
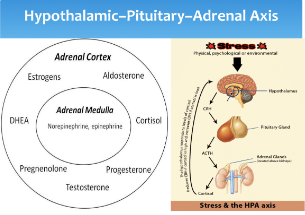
The HPA Axis: The Stress-Obesity Link
The hypothalamic-pituitary-adrenal (HPA) axis regulates stress response. Chronic trauma dysregulates this system, causing:
Elevated cortisol and adrenaline
Increased hunger and cravings for high-calorie foods
Reduced energy expenditure, making weight loss more difficult
Dysfunction of the HPA axis is associated with obesity and metabolic disorders (Rohleder, 2019).
Immune System, Metabolism, and Adrenal Fatigue
Undigested trauma weakens the immune system, making the body more susceptible to infections, inflammation, and autoimmune conditions. Chronic stress also leads to adrenal fatigue, which can cause:
Extreme fatigue
Reduced motivation for physical activity
Poor metabolic efficiency
Divergent Responses to Trauma: Weight Gain vs. Weight Loss
Not everyone responds to trauma the same way. Some individuals gain weight due to increased cortisol and insulin resistance, while others lose weight due to appetite suppression and hyperactivity of the sympathetic nervous system. Understanding these responses is essential for creating a personalized approach to healing.

Healing Strategies: More Than Just Therapy
While mental health counseling is essential for processing trauma, incorporating holistic lifestyle changes can significantly improve both physical and mental health.
Nutrition: The Mediterranean Diet and Whole Foods
A diet rich in whole, anti-inflammatory foods can help regulate hormones, support gut health, and reduce stress. The Mediterranean diet, which avoids processed foods, includes:
Healthy fats (olive oil, nuts, avocados)
Lean proteins (fish, eggs, legumes)
High-fiber vegetables and fruits
Fermented foods (yogurt, sauerkraut) for gut health
This dietary approach has been shown to lower inflammation and improve mood (Jacka et al., 2017).
Get more Nature, Pets, and Relationships in your routine.
Spending time in nature lowers cortisol and boosts mood
Interacting with pets reduces stress hormones and promotes emotional well-being
Strong relationships with loved ones provide emotional support and reduce feelings of isolation, helping to counteract stress-induced fat storage
Resistance Training and Exercise
Regular physical activity, particularly resistance training, helps:
Lower cortisol levels
Improve insulin sensitivity
Build muscle, which increases metabolic rate
Release endorphins that enhance mood and reduce stress
Studies show that strength training reduces symptoms of PTSD and anxiety while supporting metabolic health (Gordon et al., 2017).

Takeaway
Fat loss and overall health go beyond calories in vs. calories out. Past trauma plays a major role in hormonal balance, metabolism, and immune function. Addressing trauma through mental health support, proper nutrition, exercise, and holistic lifestyle strategies can help regulate the body and support long-term health.
By understanding the connection between trauma and fat loss, we can create a more effective and sustainable approach to both physical and mental well-being.
Chuck Walton
Strength coach & Nutritionist